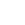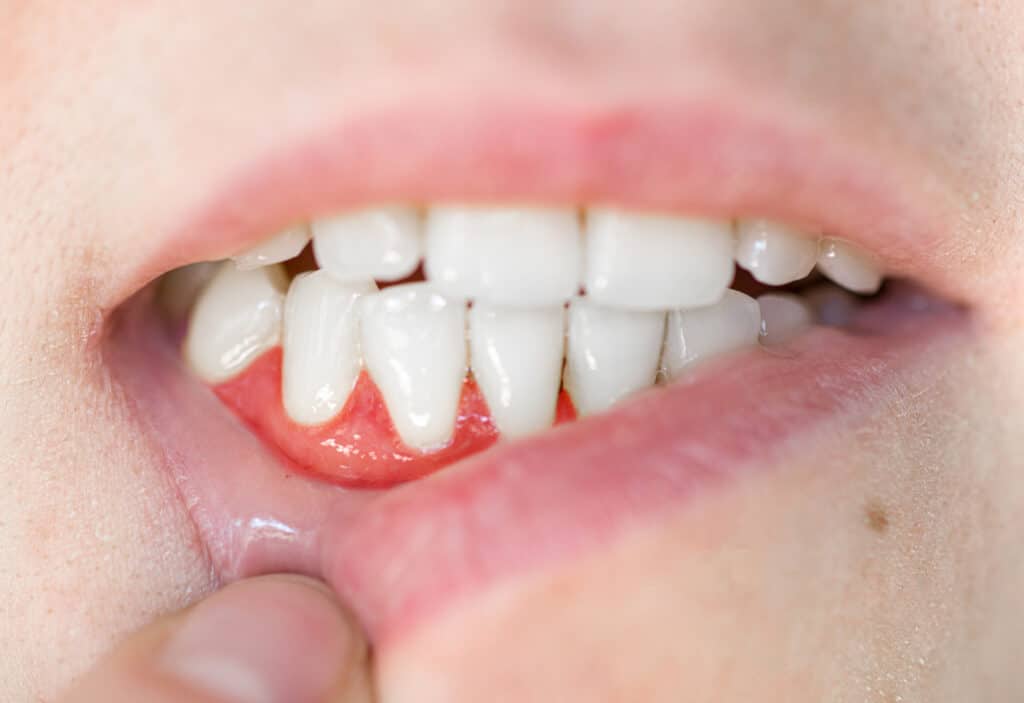
A tooth infection may begin as a small cavity or mild toothache, but if left untreated, it can quickly become a serious health concern. Oral health is closely connected to overall wellness, and infections can affect other parts of the body in many ways you may not realize.
Below, we’ll explain the risks of untreated tooth infections, so you can recognize the symptoms early and get treatment before complications develop.
What Is a Tooth Infection?
A tooth infection, also called a dental abscess, occurs when bacteria infiltrate the pulp (the inner layer of a tooth) or surrounding gum tissue and create a painful pocket of pus. This infection often develops because of untreated cavities, cracked or damaged teeth, gum disease, poor oral hygiene, or previous dental trauma.
Once bacteria reach the tooth pulp, which contains nerves and blood vessels, inflammation and infection can spread rapidly.
Common Signs of a Tooth Infection
When you recognize symptoms early, you can help keep infections from worsening. Common warning signs include:
- Persistent toothache or throbbing mouth pain
- Sensitivity to hot or cold temperatures
- Swelling in the gums or face
- Pain when chewing
- A bad taste or smell in the mouth
- Swollen lymph nodes
- Fever (100°F or higher)
- Pus drainage near the affected tooth
- Pimple-like bumps on your gums
- Unexplained fatigue or a general feeling of being unwell
Even if symptoms seem mild or temporarily improve, an infection may still be present and spreading.
How Tooth Infections Spread
The mouth contains many blood vessels, making it easy for bacteria to travel beyond the infected tooth. Without treatment, bacteria can spread into nearby tissues, the jawbone, the sinuses, and even into blood vessels.
In some cases, infections may lead to serious medical emergencies requiring hospitalization.
Increased Risk of Heart Problems
Research has revealed a connection between oral infections and cardiovascular health. Bacteria from dental infections may enter the bloodstream and contribute to inflammation in blood vessels. This may increase the risk of heart disease, stroke, and endocarditis (an infection of the heart lining).
Maintaining good oral health may support overall heart health.
Respiratory Complications
Bacteria from infected teeth and gums can sometimes be inhaled into the lungs. This may increase the risk of respiratory infections or pneumonia, especially in older adults or individuals with weak immune systems.

Impact on Diabetes Management
People with diabetes may have a harder time fighting infections, including dental abscesses. At the same time, untreated infections can make blood sugar levels harder to control, creating a cycle that affects both oral and overall health.
Regular dental care is especially important for individuals managing diabetes.
Bone and Tissue Damage
An untreated tooth infection can gradually destroy surrounding bone and soft tissues. Over time, this may lead to tooth loss, jawbone deterioration, gum recession, and facial swelling. Prompt treatment can often prevent permanent damage.
Risk of Severe Systemic Infection
In rare but serious cases, a tooth infection can spread into the bloodstream and cause sepsis, a life-threatening condition. If you have a severe infection, you may also have a high fever, rapid heart rate, difficulty breathing, severe swelling, confusion, or dizziness.
You may also develop Ludwig’s Angina, a severe bacterial infection of the mouth and neck that quicky cause a dangerous airway obstruction, a brain abscess, or a cavernous sinus thrombosis (a blod clot that forms at the base of the brain).
If you experience severe symptoms, you should seek immediate medical attention.
Treatment Options for Tooth Infections
The appropriate treatment will depend on the severity of the infection. You may need antibiotics to control the bacterial infection, a root canal to remove infected tissue, or a tooth extraction if the tooth cannot be saved.
Early intervention often allows for conservative treatment and faster recovery.
How to Prevent Tooth Infections
Preventive dental care plays an important role in protecting both your oral and overall health. You should brush twice daily with fluoride toothpaste, floss once daily, and schedule regular dental checkups and cleanings. You should also treat cavities promptly, avoid tobacco products, and limit your intake of sugary foods and drinks.
Addressing small dental issues can help prevent more serious complications later.

Don’t Ignore Pain in Your Mouth
Do not ignore tooth pain, swelling, or signs of infection. Dental problems rarely resolve on their own, and delaying treatment can increase the risk of complications affecting your overall health.
If you notice any concerning symptoms, schedule a dental evaluation as soon as possible. Prompt care can relieve discomfort, protect your oral health, and keep the infection from impacting the rest of your body.
Taking care of your teeth today ensures the rest of your body stays healthy.